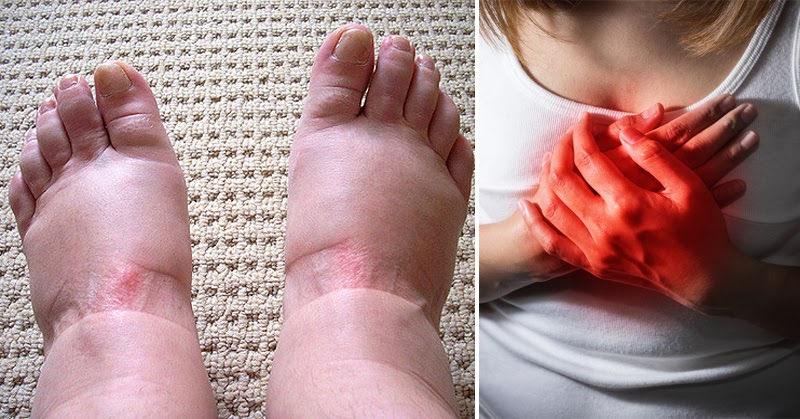
Swollen feet are common, especially as we get older, but that does not mean they should be brushed aside. Sometimes swelling comes from something simple, like standing for a long time or a warm day. Other times, it can be your body’s way of waving a red flag about your heart, kidneys, veins, or even a possible infection. Knowing the difference matters, because quick action can protect your health and keep you moving comfortably.
If you notice your shoes suddenly feel tight, your socks leave deep marks, or one foot looks much bigger than the other, it is worth paying attention. A little puffiness that fades after you elevate your legs may be harmless. Swelling that appears suddenly, worsens quickly, or comes with other concerning symptoms deserves a closer look by a healthcare professional.
This easy-to-read guide walks you through nine important warning signs linked to swollen feet that you should never ignore. Each section explains what to watch for, why it matters, and what to do next. The goal is not to alarm you, but to help you feel confident about when home care is enough and when a doctor’s visit or urgent care is the safer choice.
Deep vein thrombosis
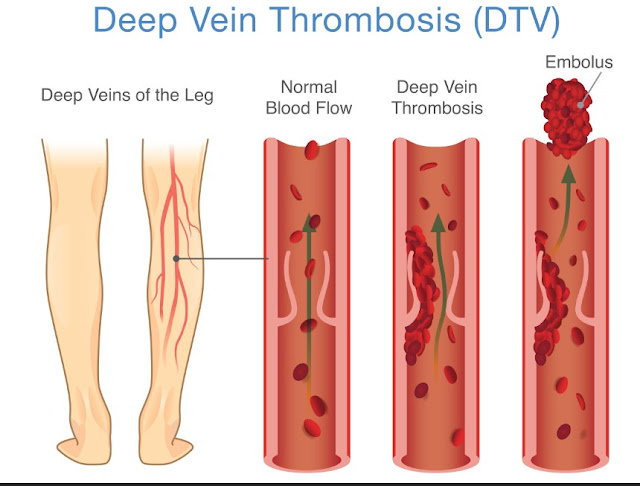
One of the most serious causes of sudden swelling in a single leg is a deep vein thrombosis, often called a DVT. This is a blood clot that forms in a deep vein, usually in the lower leg or thigh. The affected foot or ankle may swell quickly, feel warm, ache or cramp, and the skin might look red or have a bluish tint. Pressing on the calf can feel tender, and you may notice the discomfort gets worse when you stand or walk.
This is an emergency because a piece of the clot can travel to the lungs and cause a life-threatening blockage known as a pulmonary embolism. If swelling in one foot or leg appears out of the blue, especially after a long trip, recent surgery, an illness that kept you in bed, or if you have a history of clots, call your doctor right away or seek urgent care. If you also have chest pain, sudden shortness of breath, or feel faint, call emergency services immediately.
Heart strain and fluid buildup
When the heart struggles to pump efficiently, fluid can collect in the lower legs, ankles, and feet. This type of swelling often affects both feet, may be worse in the evening, and can improve overnight. You might also notice shortness of breath when walking or lying flat, needing extra pillows to sleep, fatigue, or unexplained weight gain from fluid retention. Rings may feel tighter and socks can leave deep impressions by day’s end.
These symptoms can be signs of fluid overload related to heart failure or rhythm problems. Do not ignore this pattern. If swelling is new, getting worse, or paired with breathing difficulties, call your healthcare provider promptly. Timely treatment can ease swelling, protect your heart, and help you stay active. Simple steps like elevating your legs and reducing salty foods may offer some comfort, but they should go hand-in-hand with medical guidance.
Kidney problems and fluid retention
Your kidneys act like the body’s filters, removing extra fluid and waste. If they are not working well, fluid can build up in your legs and feet, making them puffy. You may also notice swelling around your eyes in the morning, foamy urine, or a rise in blood pressure. For some people, kidney-related swelling appears gradually and is easy to miss until shoes or pant legs feel uncomfortably tight.
If you have diabetes, high blood pressure, or a family history of kidney disease, pay special attention to new or worsening foot swelling. Let your doctor know, especially if it comes with changes in urination, back pain just below your ribs, or sudden weight gain. Routine blood and urine tests can check kidney function, and early treatment can make a big difference in how you feel day to day.
Liver disease and low protein levels
The liver helps make proteins that keep fluid inside your blood vessels. When the liver is not working properly, protein levels can drop and fluid can leak into surrounding tissues, causing swelling in the ankles and feet. You might also notice a swollen belly, yellowing of the skin or eyes, dark urine, or easy bruising. While not everyone with liver issues has obvious symptoms, ankle swelling can be an early clue that something is off.
If your feet and ankles are puffy and you have a history of heavy alcohol use, hepatitis, fatty liver disease, or unexplained fatigue and loss of appetite, let your healthcare provider know. They may recommend simple blood tests and, if needed, imaging studies to check on your liver. Addressing liver health early can ease swelling and prevent bigger problems down the road.

Infection or cellulitis
Warmth, redness, tenderness, and swelling in the foot or lower leg can be signs of cellulitis, a skin and soft tissue infection that needs prompt treatment. The area may feel hot to the touch, throb, and sometimes streaks of redness can spread upward. A fever or chills can occur as your body fights the infection. Small cuts, athlete’s foot, poor circulation, and diabetes can raise the risk of infections in the feet.
If you notice a painful, red, and swollen area, especially if you have diabetes or nerve problems that reduce foot sensation, call your doctor the same day. Early antibiotics can stop the infection from getting worse. Keep the area clean, avoid squeezing or puncturing blisters, and rest with your leg elevated while you wait for care. Untreated cellulitis can spread quickly, so it is important not to delay.
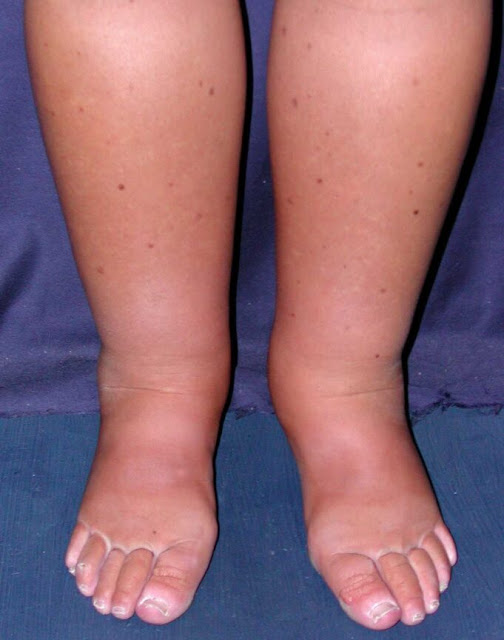
Lymphedema and heavy, persistent swelling
Lymphedema happens when the lymph system, which normally drains excess fluid, gets blocked or damaged. The result is long-lasting swelling that can make your feet and lower legs feel heavy and tight. The skin may look thick, dry, or firm, and pressing a thumb into the area might leave a brief dent early on, then later the skin can feel more rubbery. It may affect one side more than the other, especially after surgery or radiation therapy that involved the lymph nodes.
If your swelling does not go away with rest, returns day after day, or follows treatment for cancer or a major infection, talk with your doctor. Special therapy, gentle exercises, skin care, and compression garments can help move fluid and protect the skin from infections. Early attention keeps lymphedema more manageable and helps you stay active.
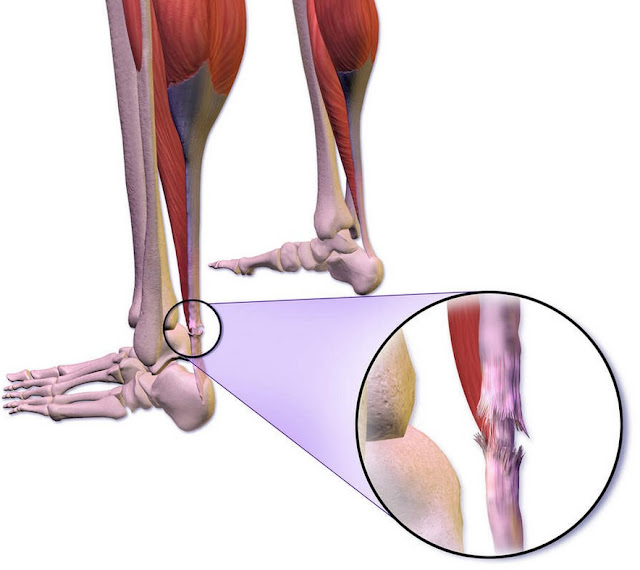
Injury, sprain, or fracture
Sometimes the cause of swelling is more straightforward. A misstep off a curb, twisting your ankle, or dropping something on your foot can lead to sudden swelling, bruising, and pain. You might notice it hurts to put weight on the foot, and the area becomes tender to touch. Even if you can walk, a bone can still be cracked or a ligament badly stretched, so it pays to get it checked if the pain or swelling is significant.
Use rest, ice, compression, and elevation soon after an injury to limit swelling and ease discomfort while you arrange an evaluation. If the shape of your foot looks unusual, if the pain is severe, or if you cannot take more than a few steps, seek prompt care. Quick diagnosis helps you heal properly and avoids long-term stiffness or repeated sprains.
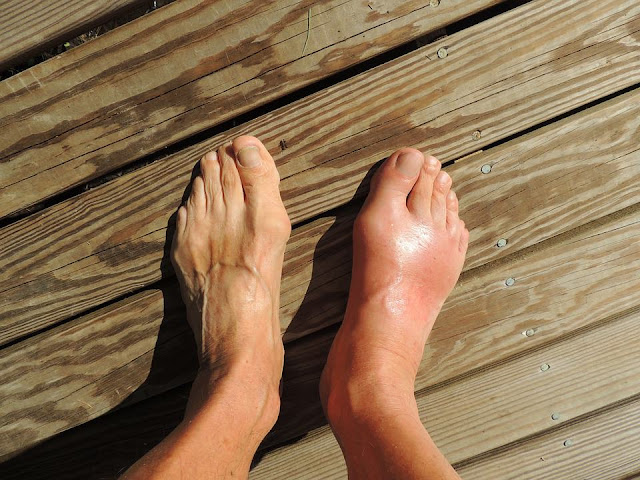
Chronic vein trouble and varicose veins
Over time, the valves inside your leg veins can weaken, allowing blood to pool in the lower legs. This is called chronic venous insufficiency, and it often goes hand-in-hand with varicose veins. Swelling tends to be worse after sitting or standing for long periods and may improve when you elevate your feet. The skin around the ankles can look darker or itch, and in more severe cases, slow-healing sores can develop near the shins or ankles.
If you notice a daily pattern of swelling that eases overnight but returns by evening, talk with your healthcare provider. Supportive stockings, regular movement, leg elevation, weight management, and procedures that improve vein function can make a big difference. Addressing vein problems early helps protect the skin and keep you on your feet comfortably.
Medication side effects
Some medicines can cause swelling in the feet and ankles by relaxing blood vessels or changing how your body holds on to salt and water. Common examples include certain blood pressure pills like calcium channel blockers, some anti-inflammatory drugs, steroids, and hormones. A few diabetes medications can also contribute. The swelling may develop gradually in both feet and might be more noticeable later in the day.
Do not stop any medication on your own, but do call your doctor or pharmacist if you suspect a new or worsening swelling started after a prescription was changed or added. There are often alternatives or dose adjustments that can help. In the meantime, simple steps like elevating your legs and moving your ankles throughout the day can offer relief.

When swollen feet are an emergency
It is wise to seek urgent care when swelling comes on suddenly in one leg, when the area is painful and warm, or when swelling is paired with chest pain, shortness of breath, coughing up blood, confusion, or fainting. These can point to a blood clot or heart and lung problems that need immediate attention. New, rapidly spreading redness with fever also calls for same-day evaluation to rule out a serious infection.
Trust your instincts. If something feels very wrong, it is far better to be checked and reassured than to wait and risk complications. Quick care can be life-saving and often prevents longer recoveries later on.
Everyday steps that can help
For mild swelling linked to heat, travel, or a long day on your feet, simple measures may bring welcome relief. Rest with your legs raised above heart level for a while to help fluid move back toward your core. Flex your ankles up and down several times an hour when sitting, and take short walking breaks to keep blood flowing. Keep shoes roomy and comfortable so they do not pinch, and choose soft socks that do not dig into your skin.
Staying hydrated, enjoying a diet with less salt, and maintaining a healthy weight also support better circulation. Over-the-counter compression socks can be helpful for some people, but they are not right for everyone. If you have poor circulation, nerve problems, or a history of clots, ask your doctor which level of compression is safe before you try them.
How doctors figure out the cause
Your healthcare provider will start by asking when the swelling began, whether it is in one foot or both, and what makes it better or worse. They will look for clues on your skin such as color changes, warmth, or tenderness, and they might check your heart, lungs, blood pressure, and weight. Depending on what they find, they may order blood tests to check kidney, liver, and heart function, an ultrasound to look for a blood clot or vein problems, or an X-ray if an injury is suspected.
The right diagnosis leads to the right treatment. For example, a DVT may be treated with blood thinners, while heart-related fluid overload might call for diuretics and adjustments in heart medicines. Infections are treated with antibiotics, and injuries often do best with rest and guided rehabilitation. When medicines cause swelling, a change in prescription can bring quick improvement.
A quick word on prevention
Small habits add up. Keeping active with daily walks, gentle stretches, and ankle movements helps your calves pump blood back toward your heart. Taking breaks from long periods of sitting or standing, propping your feet on a stool while relaxing, and maintaining good control of blood pressure, blood sugar, and cholesterol all support healthier feet and legs. Managing skin and nail care, especially if you have diabetes, lowers the risk of infections that can lead to swelling.
If you have a big trip coming up, plan ahead. Wear comfortable shoes, move your ankles often, stand and stretch when it is safe to do so, and drink water regularly. If you have a known risk of blood clots, talk with your doctor about any extra steps before you travel.
The bottom line
Swollen feet can be a simple annoyance or a sign that deserves quick attention. Pay special care to swelling that is sudden, affects one foot more than the other, comes with pain, warmth, redness, shortness of breath, chest discomfort, fever, or any rapid change in how you feel. The sooner you check in with a healthcare professional, the sooner you can get the right care—and the sooner your feet can feel like themselves again.
Your body speaks to you in many ways. By learning what your feet are trying to say and acting promptly when something seems off, you protect your health today and keep yourself moving comfortably for many years to come.