Why swollen feet deserve your attention
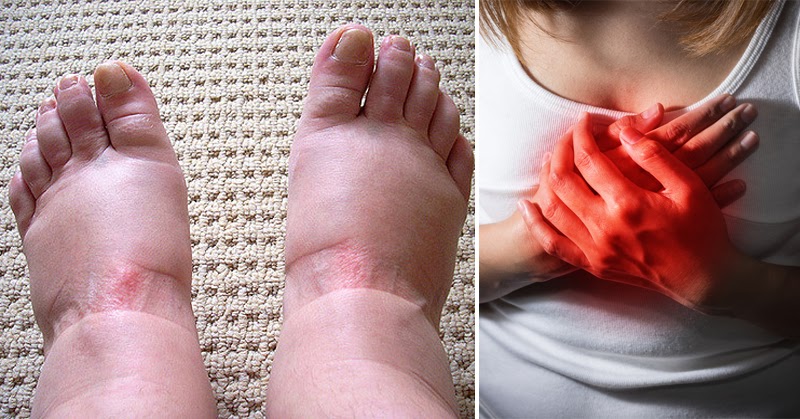
Swollen feet are common, especially as we get older, after a long day on our feet, during hot weather, or following travel. Most of the time the swelling eases with rest, elevating the legs, and a glass of water. But sometimes puffy feet or ankles are your body’s way of waving a red flag. Recognizing when swelling is more than a nuisance can help you act early, avoid complications, and feel better faster. This friendly guide explains nine important reasons feet may swell, how each one tends to feel and look, and what steps you can take. If something here sounds like you, it’s a good idea to talk with your healthcare professional. And if your swelling comes on suddenly, is only on one side, or is paired with chest pain, shortness of breath, or new confusion, treat it as urgent and get medical help right away.
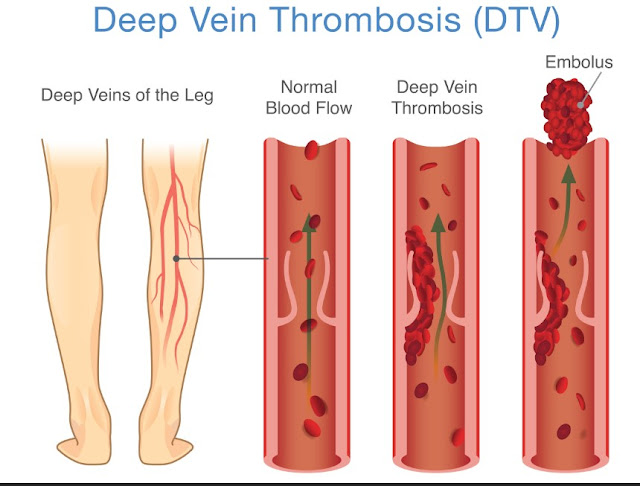
Deep vein thrombosis
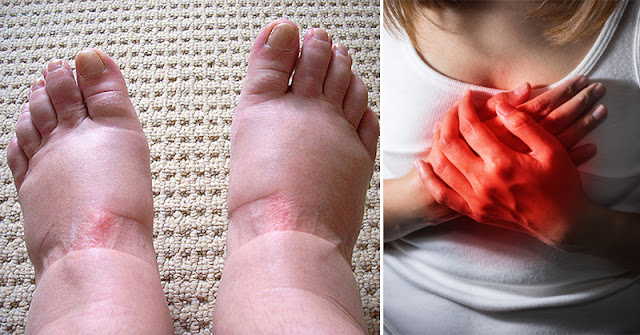
A deep vein thrombosis, often called a DVT, is a blood clot that forms in a deep vein, most commonly in the calf or thigh. It can block normal blood flow and push fluid into nearby tissues, causing one leg or foot to swell more than the other. The swelling may appear suddenly, and the area can feel heavy, warm, tender, or painful, especially when you stand or walk. The skin might look reddish or slightly blue. A DVT is serious because part of the clot can break off and travel to the lungs, which is a life‑threatening emergency. If you notice new one‑sided leg or foot swelling, particularly after surgery, an illness, a long car or plane ride, or a period of being less active, treat it as urgent and seek medical care. Doctors can confirm a DVT with an ultrasound and begin treatment that helps prevent complications and protects your health.
Heart strain and heart failure
Your heart works like a pump. When that pump is under strain and cannot move blood as effectively, fluid can collect in the lowest parts of the body, most noticeably in the feet and ankles by late afternoon or evening. Swelling from heart issues may be in both feet, and pressing a finger into the swollen area can leave a temporary dent, a sign called pitting. You might also notice shortness of breath when lying flat, waking up at night needing air, fatigue, a racing or irregular heartbeat, or unexpected weight gain from fluid. If your shoes feel tighter most days, and you are noticing breathlessness or a persistent cough, let your clinician know. Early care, including reviewing medications, limiting excess salt, elevating your legs, and gentle activity as advised, can make a big difference in how you feel and help you stay active and independent.
Kidney troubles and fluid buildup
Our kidneys balance fluids and salts. When they are not working as well, extra fluid may collect in the body and show up first as swelling around the feet and ankles, and sometimes puffy eyelids in the morning. You might also see changes in urination, such as going more or less than usual, foamy urine, or darker color. Tiredness, loss of appetite, and muscle cramps can appear as kidney function declines. If your swelling is steady and you also have a history of high blood pressure, diabetes, or kidney disease, it is wise to ask your healthcare professional for a checkup. Simple blood and urine tests can offer clarity. Managing salt intake, keeping blood pressure and blood sugar in range, and reviewing any medications that affect the kidneys can help. The goal is to protect kidney function while easing the discomfort and tightness you feel in your shoes and socks.
Liver disease and ankle swelling
The liver makes proteins that help keep fluid inside blood vessels. When the liver is inflamed or scarred, as in hepatitis or cirrhosis, these proteins can be low and fluid may leak into tissues, leading to swelling in the feet and ankles. People may also notice fullness in the belly from fluid, tenderness under the right ribs, yellowing of the skin or eyes, or easy bruising. If you have a history of liver problems or heavy alcohol use and your lower legs are getting puffier, it is important to discuss it with your clinician. They may adjust medicines, recommend vaccinations, or suggest diet changes that ease liver strain. Reducing salt, staying up to date on screenings, and taking medications only as prescribed can help reduce swelling and protect liver health. The earlier these issues are identified, the more options you have to feel better and stay active.

Chronic venous insufficiency
Leg veins carry blood back to the heart using one-way valves and the squeeze of your calf muscles when you walk. If those valves weaken, blood can pool in the lower legs. This is called chronic venous insufficiency, and it often shows up as aching, a heavy feeling, and swelling that is worse by evening and improves overnight. The skin around the ankles can become itchy, darker, and more fragile over time, and varicose veins may be visible. Gentle, regular walking, elevating your legs above heart level a few times a day, and well-fitted compression socks can help the veins move blood upward. If the skin is changing or you’ve had sores near your ankles that heal slowly, it’s important to see a clinician. They can recommend treatments that improve circulation and reduce the risk of complications, helping you stay comfortable on your feet for the long run.
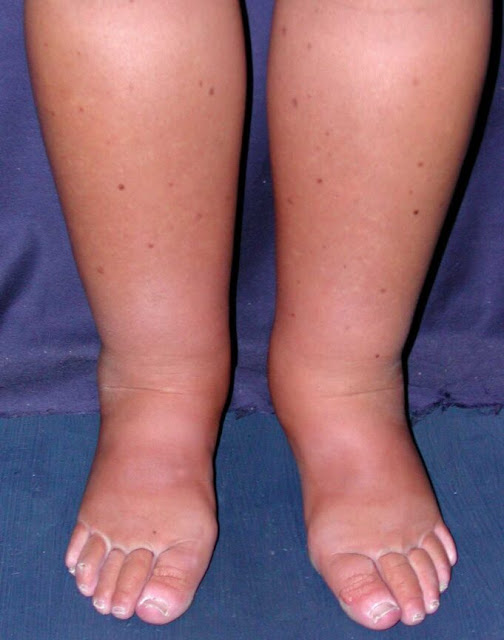
Lymphedema and firm swelling
Lymph fluid helps clear waste and fight infection. When lymph channels are damaged or blocked, fluid can collect and cause lymphedema. This swelling is often firm rather than squishy, may affect the top of the foot and toes, and does not always improve much overnight. Shoes may feel tight, and the skin can feel thick or tight like a glove that is hard to take off. This sometimes follows surgery, radiation, or infections, and it can also occur without a known cause. Gentle movement, careful skin care, and specialized compression garments prescribed by a professional can help move fluid and protect the skin. A lymphedema therapist can teach safe techniques to reduce swelling and keep you active. Because skin in swollen areas is more vulnerable to infection, it is important to moisturize daily, treat small cuts promptly, and contact your clinician if you notice redness, warmth, or fever.
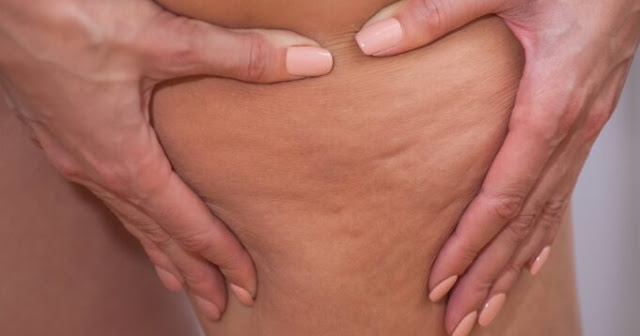
Infection or cellulitis
Red, hot, tender skin on the foot or lower leg that swells quickly may be a skin infection called cellulitis. It often starts from a small cut, scrape, or athlete’s foot opening a pathway for bacteria. The area can feel tight, sore to the touch, and may be paired with fever or chills. People with diabetes, circulation problems, or lymphedema are at higher risk. Cellulitis needs prompt medical treatment because it can spread quickly. If you think you may have an infection, contact your healthcare professional the same day. To help prevent infections, wash and dry your feet daily, moisturize to avoid cracks, trim nails carefully, wear well‑fitting shoes, and check your feet regularly for blisters or cuts. Catching infections early means faster recovery and less chance of complications that keep you off your feet. After treatment, continue good foot care to protect the skin barrier.
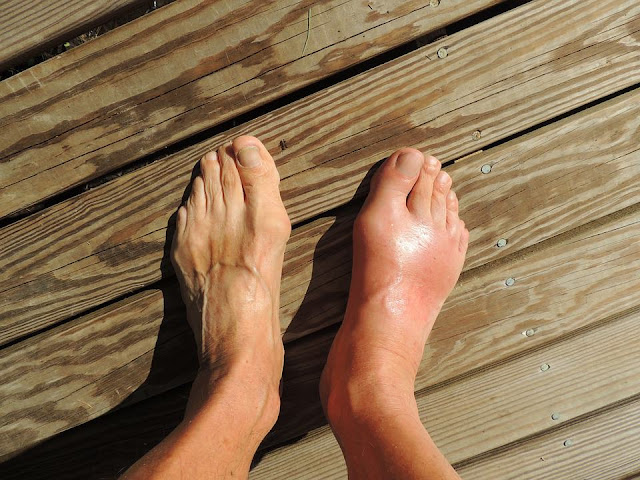
Injury, sprain, or fracture
Not all swelling is medical in nature. A misstep on a curb, a twist in the yard, or a stumble on the stairs can strain ligaments or even cause a small fracture. Injuries often cause swelling that comes on quickly, with bruising, tenderness, and pain when putting weight on the foot or ankle. Resting, icing for short periods, gentle compression, and elevating the foot can help in the first two days. If you cannot put weight on the foot, the shape looks unusual, the pain is severe, or the swelling does not improve, it is time to be checked. An X‑ray can rule out a break. Early support, such as a brace or walking boot when needed, speeds healing and reduces the chance of long‑term stiffness. Good, sturdy shoes with proper support and watching for trip hazards at home can help prevent the next tumble.
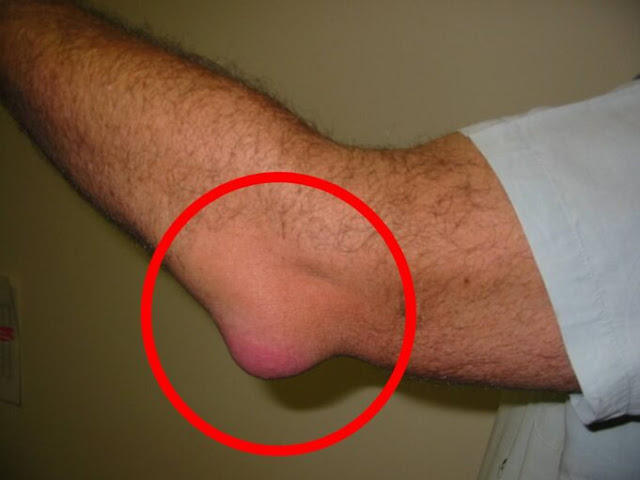
Medication side effects
Some common medicines can cause the body to hold onto fluid, especially around the feet and ankles. Drugs for blood pressure such as certain calcium‑channel blockers, some diabetes medicines, anti‑inflammatories taken for pain, hormones, and even over‑the‑counter remedies may contribute to swelling. If your feet began to puff up soon after starting a new medication, or after a dose change, make a note of the timing. Do not stop a prescription on your own, but do call your clinician or pharmacist to review your list and discuss options. Sometimes a small adjustment or switching to a different medicine eases swelling without sacrificing the benefits of treatment. While you are sorting it out, simple steps like propping your feet on a pillow when resting, moving your ankles in circles during the day, and wearing roomy, supportive shoes can help you stay comfortable.

Thyroid and hormonal changes
Low thyroid function can slow many body processes, leading to tiredness, weight changes, dry skin, and a tendency to hold onto fluid. The swelling from an underactive thyroid is often mild and may come with a feeling of stiffness in the legs and feet. Other hormonal shifts, such as those related to menopause, can also influence how the body manages salt and water. If your feet are a little puffy and you also notice sensitivity to cold, hair changes, or unexplained fatigue, it is worth asking your clinician about a thyroid check. Simple blood tests can confirm how your thyroid is doing and whether treatment is needed. Addressing thyroid balance can improve energy, comfort, and overall well‑being, and it may help your shoes feel more comfortable by the end of the day. Paying attention to these small clues can help you catch changes before they become bigger problems.
What you can do today to feel better
There are practical steps you can start right now to ease swollen feet. When you sit, take a few moments to elevate your legs so your feet are above your heart if possible; even a stack of pillows can help. Move your ankles up and down and make gentle circles several times a day to encourage circulation. On days you are able, short walks around the house or outside provide a natural calf‑muscle pump that pushes fluid back toward the heart. Choose supportive shoes that allow room for swelling, and avoid tight socks that leave deep marks. Keep your skin moisturized to prevent cracks and watch for any new redness or sores, especially if you have diabetes or vein problems. If your healthcare professional recommends compression socks, make sure they are the right strength and fit, and put them on in the morning when swelling is lowest.
When it is time to call the doctor
Swelling that is new, unexplained, or steadily getting worse deserves a call. Let your clinician know if it is on one side only, came on suddenly, or is paired with symptoms like shortness of breath, chest pain, a racing heartbeat, fever, chills, or new confusion. These signs can point to conditions that need same‑day attention. If you are managing a long‑term condition such as heart, kidney, liver, or vein disease, keep a simple daily note of your weight and how your legs look and feel. Small changes can help your care team adjust treatment before swelling becomes uncomfortable. Most importantly, trust your instincts. You know your body best. A quick conversation can bring peace of mind, and early care can prevent complications that limit your independence. With the right plan, most people find real relief and get back to the activities they enjoy.
The bottom line
Swollen feet are not just a cosmetic issue. They are often your body’s way of asking for attention. From blood clots and heart or kidney issues to vein problems, lymphedema, infections, injuries, medications, and hormonal shifts, there are many possible reasons your shoes may feel tighter. The good news is that there are effective ways to feel better, from simple home measures to medical treatments tailored to your needs. If your swelling is new, painful, or accompanied by other concerning symptoms, reach out for help promptly. If it is part of a pattern you have noticed for a while, schedule a checkup and bring notes about when it is worse, what helps, and what else you are feeling. Together with your healthcare professional, you can uncover the cause, choose the right steps, and keep moving comfortably and confidently through your day.