A gentle, practical guide to easing gout and protecting your joints
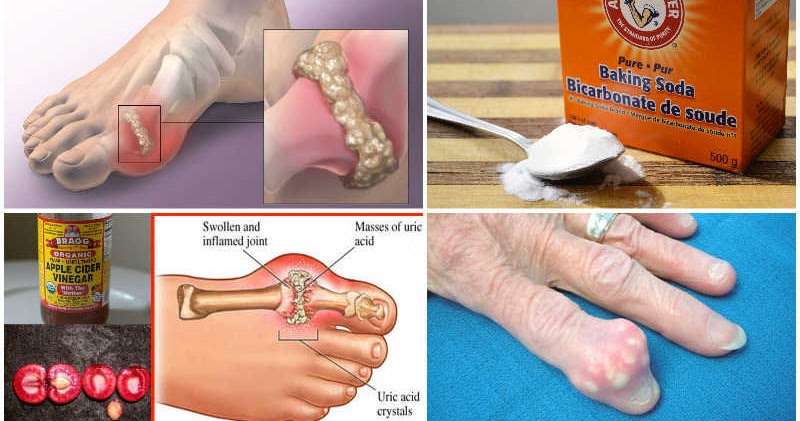
If you have ever felt a toe, foot, ankle, or finger suddenly become hot, swollen, and painfully tender, you know how much a gout flare can disrupt your day. Many people search for a quick fix to remove uric acid crystals and make the pain stop. While there is no instant switch that dissolves crystals on the spot, there are clear, effective steps you can take to calm a flare faster and reduce the chances of it returning. This guide explains those steps in plain language so you can feel more in control of your health.
Think of this as a roadmap. Some actions offer comfort and relief right away, while others steadily lower uric acid over time so crystals are less likely to form. Used together, they help you feel better now and protect your joints in the years ahead.
What uric acid crystals are and why they hurt
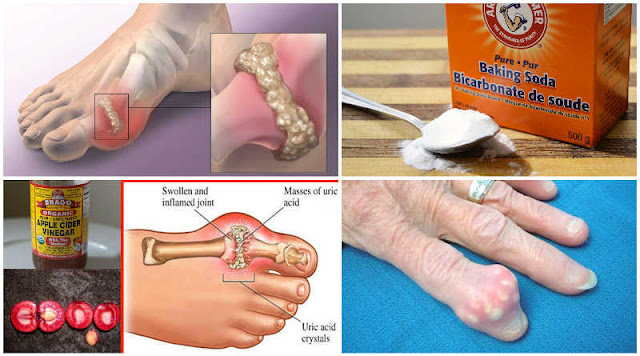
Uric acid is a natural waste product our bodies make when we break down purines, which are found in our cells and in some foods. Your kidneys filter uric acid and remove most of it in urine. When blood levels get too high for too long, tiny needle-like crystals can form inside joints and the surrounding tissues. Those crystals irritate the joint lining and trigger a powerful inflammatory response, which is what causes the redness, swelling, heat, and severe pain of a gout attack.
This means there are two linked goals. During a flare, you want to calm inflammation and protect the joint so you can move comfortably. Between flares, you want to lower uric acid levels to prevent new crystals from forming and help existing deposits shrink. Both goals are achievable with the right daily habits and, when needed, the right medication plan from your clinician.
What “quickly remove crystals” really means
It is important to set realistic expectations. Crystals do not simply flush away overnight. However, your body can stop inflammation quickly with the right care, and over weeks to months, lower uric acid levels allow crystals to dissolve and clear. The quickest wins come from soothing the flare, staying well hydrated, and avoiding common triggers. The long-term wins come from consistent routines and, if appropriate, medications that keep uric acid in a healthy range.
So the process has two speeds. Relief now focuses on reducing pain and swelling. Prevention focuses on steady, lasting changes that make future flares far less likely. Together, they add up to fewer painful days and healthier joints.
How to feel better during a flare
When a flare begins, protect the joint and give your body a calm, steady environment to ease inflammation. Rest the affected area and keep it elevated when you can. Cool compresses or a wrapped ice pack for short periods can help reduce heat and swelling. If a specific shoe or tight sock is pressing the joint, switch to something soft and roomy to avoid extra irritation.
Stay hydrated by sipping water regularly. Gentle hydration helps your kidneys clear uric acid and keeps your whole system balanced. Avoid alcohol during a flare because it can raise uric acid and slow recovery. If you have medications prescribed for flares, such as anti-inflammatory tablets recommended by your clinician, take them as directed. If you do not have a plan yet, this is a good time to call your health professional and ask about options for both immediate relief and longer-term prevention.
How to lower uric acid over time
Between flares, the goal is to keep your blood uric acid level low enough that crystals cannot form easily and existing deposits can gradually shrink. Many people reach this goal through a combination of everyday habits and, in some cases, long-term medications that control uric acid production or increase its removal. Your clinician can measure your uric acid level with a simple blood test and help you set a personal target, often below the point where crystals can form.
Progress is steady rather than sudden. Think of it like gently letting air out of a balloon. With consistent steps, pressure on the joints eases, flares become less frequent, and comfort improves.
The role of hydration
Good hydration is one of the simplest ways to support healthy uric acid levels. Water helps your kidneys do their job and prevents uric acid from becoming too concentrated. Keep a glass or bottle nearby and sip through the day, especially in warm weather or when you are physically active. Herbal teas without added sugar can count toward your fluids as well. If you take a diuretic or have heart or kidney conditions, ask your clinician about a fluid plan that is right for you.
Food choices that support healthy uric acid
Your overall eating pattern matters more than any single meal. A balanced, mostly plant-forward approach tends to help. Colorful vegetables, fruit in reasonable portions, whole grains, beans and lentils in amounts your body tolerates, nuts and seeds, and low-fat dairy can fit well into a gout-friendly plan. These foods provide fiber, vitamins, and minerals that support steady energy and overall health.
Protein is important, too. Many people do well with moderate portions of fish and poultry, along with plant proteins like tofu and lentils. If you notice a particular food seems to trigger your flares, make a note and discuss it at your next appointment. Everyone is a little different, and a simple food-and-symptom journal can be surprisingly helpful.
Foods and drinks to limit
Some foods can raise uric acid more than others. Organ meats such as liver and sweetbreads are especially high in purines and are best avoided if you have gout. Large portions of red meat and certain kinds of seafood like anchovies, sardines, mussels, and scallops may also contribute for some people. Sugary drinks and snacks, especially those sweetened with high-fructose corn syrup, can nudge uric acid higher by changing how the body processes purines. Alcohol can be a trigger as well, particularly beer and spirits, which can increase uric acid production and reduce how much you excrete.
If you enjoy these foods, consider them occasional rather than everyday choices. When you do have them, keep portions small and balance the rest of your meals with vegetables, whole grains, and low-fat dairy. Many people find they can still enjoy a wide variety of foods by being mindful of frequency and portion size.
Supportive choices that may help
Some everyday items are linked with a modest improvement in uric acid levels for many people. Low-fat dairy products such as milk and yogurt appear to promote uric acid excretion. Coffee, in moderate amounts and without added sugar, is associated with a lower risk of gout in some studies, though it is not a treatment on its own. Vitamin C from foods like oranges, berries, and peppers supports overall health and may have a small effect in lowering uric acid. If you are considering a vitamin C supplement, talk with your clinician first to make sure it is appropriate for you and your medications.
Cherries and cherry juice are often discussed in relation to gout. Some people report fewer flares when they include cherries regularly. The effect, if any, is usually modest, and results vary from person to person. It can be reasonable to include cherries as part of an overall healthy eating plan, but they are not a substitute for medical care when needed.
Weight, movement, and joint comfort
Carrying extra weight can raise uric acid levels and place more stress on your joints. Even a gradual, modest weight loss can make a meaningful difference in reducing flares and improving mobility. Aim for slow, steady progress by focusing on nourishing foods and daily movement that you enjoy and can sustain, such as walking, swimming, or gentle cycling. During a flare, rest the affected joint, but as the pain settles, return to comfortable activity to keep your muscles and joints strong.
If you are starting a new exercise plan or have other health conditions, discuss your ideas with your clinician. A small change you like and can stick with is much more powerful than a perfect plan you only follow for a week.
Medications that prevent crystals
For many people, long-term medicines that lower uric acid are the most reliable way to prevent gout attacks and dissolve existing crystals. These medicines either reduce the amount of uric acid your body makes or help your kidneys remove more of it. Your clinician will consider your health history, kidney function, and current medications to choose the safest option and dose for you.
It is common to take an additional protective medicine for a short time when starting a uric acid–lowering drug, because as crystals begin to soften and shift, they can briefly trigger flares. This does not mean the medicine is failing. It is a sign that deposits are changing, and with guidance, the short-term flares usually pass as your uric acid stays in the target range.
Medications that treat flares
When a flare strikes, anti-inflammatory medicines can be very effective at easing pain and swelling. Several types are available, and your clinician can recommend one that fits your health needs, especially if you have heart, kidney, or stomach concerns. The key is early treatment at the first sign of a flare and following the plan you have been given. If you do not yet have a flare plan, ask for one so you are prepared.
Never start or stop prescription medicines without talking to your health professional. If you use over-the-counter pain relievers, read labels carefully and check for interactions with your regular medications.
Managing other health conditions
Gout often travels with other conditions such as high blood pressure, kidney disease, diabetes, and heart disease. Treating these conditions well helps your whole body and can make gout easier to control. If you take a water pill or other medicines that may raise uric acid, your clinician can discuss options and adjust your plan if appropriate.
Regular checkups and simple blood tests give you a clear picture of how you are doing. Knowing your uric acid number is like knowing your blood pressure or cholesterol. It helps you and your care team tailor your plan and celebrate progress.
What to do if flares keep returning
If you are having repeated flares, do not lose heart. Persistent attacks usually mean your uric acid level has not stayed low enough for long enough. A small change in medication dose, a fresh look at triggers, or renewed focus on hydration and daily habits can turn the tide. Keep notes on what you eat, drink, and do during the days before a flare. Patterns often appear that make the next step clearer.
When pain is severe, a joint becomes very red and hot, or you develop a fever or feel unwell, seek medical care promptly. Symptoms that seem like gout can sometimes be caused by infection or other conditions that need urgent attention. It is always better to check and be safe.
Myths and facts, simply explained
One common myth is that gout only affects people who overindulge. In truth, genetics, kidney function, and other health conditions play a big role. Lifestyle matters, but it is only one piece of the puzzle. Another myth is that a single superfood or drink can wash away crystals overnight. While certain foods can help and others can hinder, gout responds best to a steady, combined approach of healthy routines and, when needed, the right medications.
A helpful fact to remember is that gout is very manageable. With today’s knowledge and treatments, most people can reduce flares dramatically and protect their joints from long-term damage. Step by step, you can get there.
A simple day that supports lower uric acid
Picture an ordinary day arranged to be kind to your joints. You start your morning with water and a balanced breakfast, perhaps yogurt with fruit and a sprinkle of nuts or a vegetable omelet with whole-grain toast. You enjoy a cup of coffee if you like, without a lot of sugar. Midday, you take a comfortable walk or do gentle stretches, and you keep sipping water throughout the day. Supper features vegetables, a modest portion of lean protein, and a whole grain like brown rice or barley. If you want something sweet, a small bowl of berries can be satisfying without pushing uric acid up.
As bedtime approaches, you make sure any prescribed medicines are taken as directed, and you set out a glass or bottle of water for tomorrow. None of these steps is dramatic on its own, but together they create an environment where uric acid stays in a safer range and your joints stay calmer.
Working with your care team
Your health professional is your partner in this process. Ask about testing your uric acid level, setting a personal target, and choosing a plan that fits your life. If something in your plan is hard to follow, say so. There are usually several ways to reach the same goal, and a small adjustment can make a big difference in how easy it feels.
If you travel, change routines, or start a new medication for another condition, let your clinician know. Staying in touch helps prevent surprises and keeps your gout plan aligned with the rest of your health care.
Encouragement for the road ahead
It is understandable to wish for a quick cure when you are hurting. While there is no instant eraser for uric acid crystals, there is a clear, dependable path to fewer flares and better comfort. Calm the joint during a flare, hydrate well, be mindful of common food and drink triggers, and consider long-term uric acid–lowering treatment if your clinician recommends it. Over time, crystals shrink, pain fades, and confidence returns.
Every step you take, no matter how small, helps your body move toward balance. With patience and a good plan, you can protect your joints, stay active, and enjoy your days with far less worry about gout.