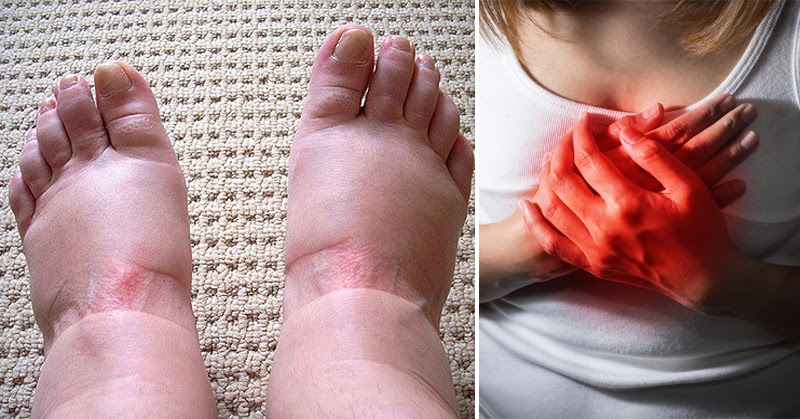
Swollen feet are common, especially after a long day of sitting, standing, or traveling. For many people, mild puffiness that fades overnight is simply the body holding on to a little extra fluid. But sometimes swelling is your body’s way of waving a red flag and asking for attention.
Understanding what your swelling might mean can help you decide when simple rest is enough and when it is time to call your healthcare provider. The goal is not to worry you, but to guide you. When you know the warning signs, you can act sooner, feel better faster, and protect your long-term health.
Below are nine important reasons feet and ankles swell that deserve a closer look. Each section explains what to watch for, why it happens, and what kind of action makes sense. If anything here sounds familiar, trust your instincts and reach out for care.
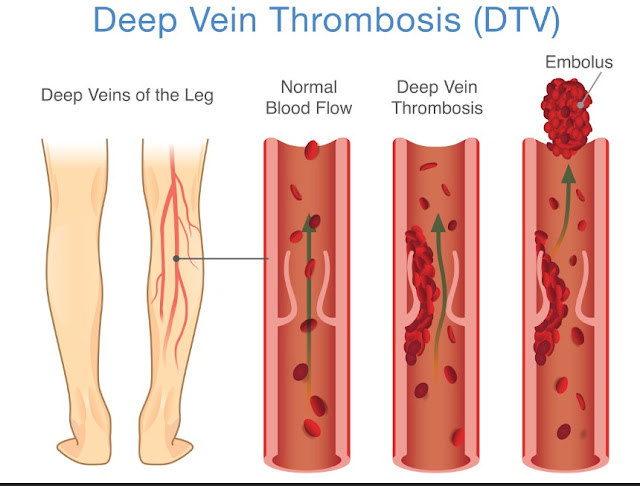
Deep vein thrombosis
Deep vein thrombosis is a blood clot that forms in a deep vein, most often in the calf or thigh. It can block blood flow and trap fluid in the lower leg and foot, which leads to sudden swelling. The danger is that part of the clot can break loose and travel to the lungs, a medical emergency.
Warning signs include swelling that affects one leg more than the other, new calf pain or tenderness, warmth, and a reddish or bluish color to the skin. The swelling may appear quickly over hours, and your shoe on that side can feel tight even if it fit fine the day before.
Risk is higher after recent surgery, long flights or car rides, a period of bed rest, cancer treatment, hormone therapy, smoking, or a prior clot. If swelling comes with chest pain, coughing up blood, a racing heartbeat, dizziness, or sudden shortness of breath, seek emergency help immediately.
If you have the warning signs without trouble breathing, contact your clinician the same day. A quick ultrasound can usually confirm the diagnosis, and treatment can prevent serious complications.
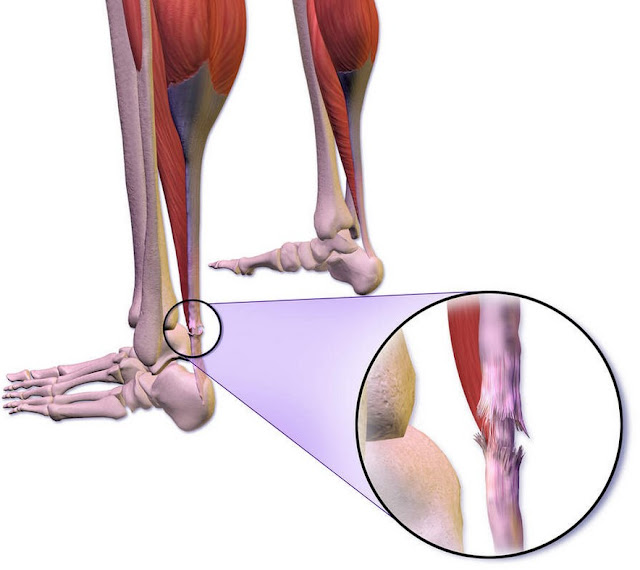
Poor leg vein circulation
Poor leg vein circulation, often called chronic venous insufficiency, happens when the one-way valves in your leg veins get weak or damaged. Instead of sending blood smoothly back to the heart, some of it slips backward and pools around the ankles and feet. By evening, shoes and socks can feel uncomfortably tight.
You may notice aching, heaviness, cramping, or itching in the lower legs. Skin can darken around the ankles, and small wounds in that area may heal slowly. Varicose veins are common and can go hand in hand with this kind of swelling.
Gentle movement, calf exercises, and putting your feet up for 20 to 30 minutes can help. Compression socks may also reduce swelling, but check with your healthcare provider first, especially if you have heart disease, peripheral artery disease, or nerve problems from diabetes. If skin changes, sores, or significant pain appear, schedule an appointment for tailored treatment.
Heart problems and fluid overload
The heart is a powerful pump. When it gets tired and cannot move blood as strongly as it used to, fluid can back up into the legs and feet. This is often called congestive heart failure. It tends to cause swelling in both legs rather than just one.
Clues that point to the heart include weight gain over a few days, swelling that rises above the ankles, tight rings or a puffy belly, and shortness of breath with activity or when lying flat. Waking at night feeling breathless is another red flag that fluid may be building up.
If you notice these changes, contact your clinician promptly. Medication adjustments, reducing salt, and checking your kidneys and electrolytes can make a big difference. Seek urgent help if shortness of breath is severe, if you feel faint, or if chest discomfort accompanies the swelling.
Kidney strain or kidney disease
Healthy kidneys act like your body’s filter, removing extra salt and water. When kidneys are under strain, fluid can build up and settle in soft tissues, including the feet and ankles. Swelling from kidney issues may also appear around the eyes, especially in the morning.
Other hints include foamy urine, changes in how often you urinate, fatigue, nausea, and higher blood pressure. People with diabetes, high blood pressure, or a history of frequent pain reliever use are at higher risk for kidney problems.
If you suspect your kidneys are involved, ask for a simple set of tests. Blood work and a urine sample can check how well your kidneys are doing. Early care can prevent complications and ease swelling.

Liver disease and low blood protein
Your liver produces important proteins that help keep fluid inside your blood vessels. When the liver is injured and cannot make enough of these proteins, fluid can leak into the legs, feet, and belly. Long-standing alcohol use, hepatitis, and fatty liver are common causes.
Signs that point toward the liver include yellowing of the skin or eyes, easy bruising, itchy skin, a swollen abdomen, and loss of appetite. Foot and ankle swelling from liver disease often appears along with these other symptoms.
If you have risk factors or notice these changes, set up an appointment. Gentle care of the liver, nutrition support, and medicines can help control fluid and protect your health.
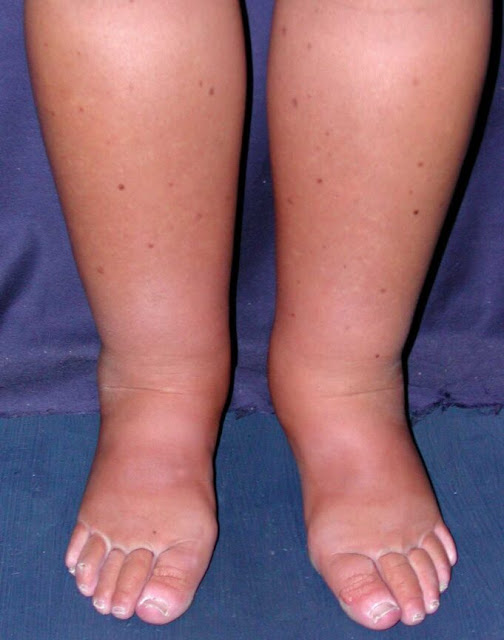
Lymphedema
Lymphedema is swelling caused by a slowdown in the lymph system, the body’s natural drain for extra fluid and waste. It can follow surgery or radiation for cancer, a severe infection, or it can be present from birth. The swelling is often firm, not easily dented with a fingertip, and may involve the toes.
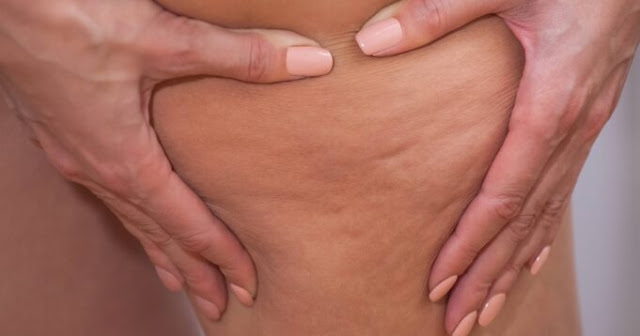
Skin over the area can feel thick or tight and may look like an orange peel. Because the skin is stretched, it can crack more easily, which raises the risk of infection. Gentle skin care and quick attention to even small cuts or bites are important.
Lymphedema responds best to specialized therapy, which may include manual lymph drainage, custom compression wraps, exercise, and careful skin care. If you notice steadily worsening swelling or frequent infections, ask your clinician for a referral to a lymphedema therapist.
Skin and soft tissue infection
When bacteria enter through a small cut, crack, or fungal rash, the skin and tissues underneath can become infected, a condition called cellulitis. One leg quickly becomes red, warm, swollen, and tender. Fever, chills, or feeling unwell often follow.
Cellulitis needs prompt antibiotics to stop it from spreading to the bloodstream. If the redness is spreading, you have a fever, or you have diabetes, seek urgent care the same day. Quick treatment usually brings fast relief and prevents complications.
To lower your risk, keep feet clean and dry, moisturize dry skin, trim toenails carefully, and treat athlete’s foot promptly. If you notice a sore that is not healing, especially near the ankle, have it checked.
Medication side effects
Some medicines make the body hold on to fluid, especially around the ankles. Common culprits include certain blood pressure pills such as calcium channel blockers, anti-inflammatory pain relievers, steroids, hormones, and a few medicines for diabetes or mood. Swelling from medication is often painless and appears in both feet.
If your swelling began soon after a new prescription or a dose change, call your clinician or pharmacist. Never stop a heart or blood pressure medicine on your own. In many cases, a small adjustment, a different time of day, or switching to another option solves the problem.
Let your care team know about all the remedies you take, including over-the-counter pills and supplements. The full picture makes it easier to find the cause and the fix.
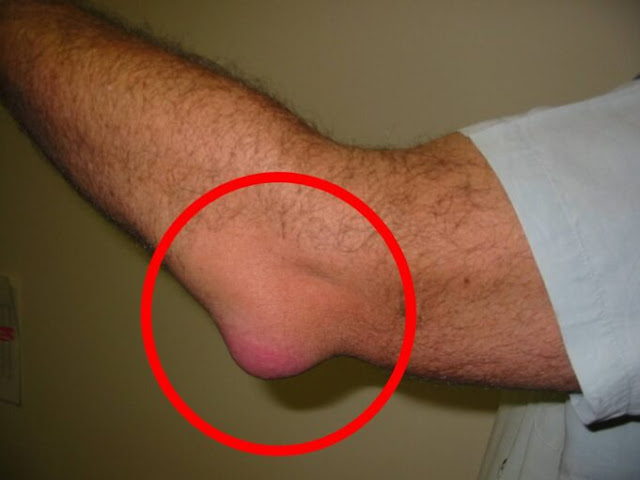
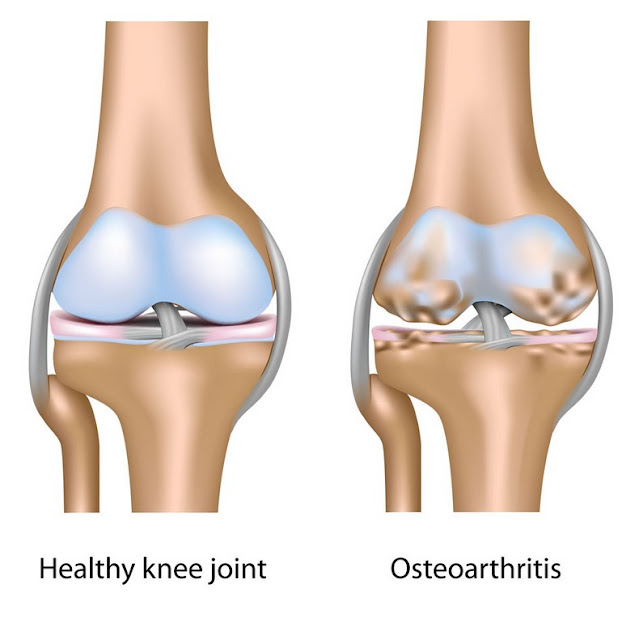
Injury, gout, or arthritis flare
An ankle sprain, overuse, or a small fracture can trigger swelling that makes it hard to fit into your shoes. The area may be bruised and tender. If you recall a twist or stumble or you feel sharp pain with each step, an X-ray or exam can rule out a break and guide treatment.
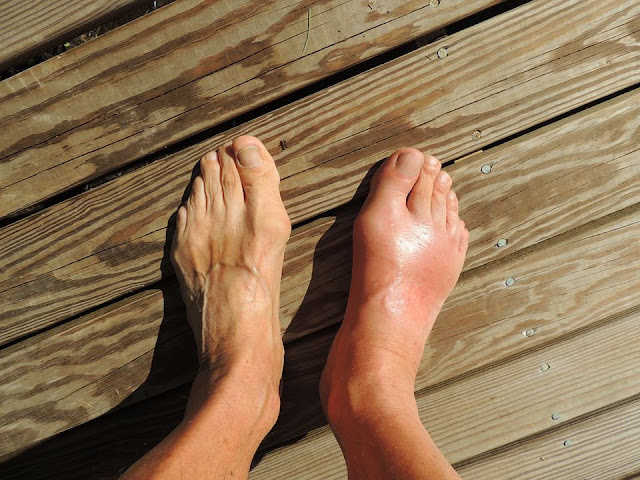
Gout is another cause of dramatic swelling and pain, often striking the big toe or midfoot at night. The joint becomes hot, very tender, and red. People sometimes describe the weight of a sheet as unbearable. Early treatment calms the flare and protects the joint from damage.
Other forms of arthritis, including osteoarthritis and rheumatoid arthritis, can also cause swelling during a flare. If a joint is red, hot, and you have a fever, seek urgent care to check for an infected joint, which needs immediate attention.

When to get care right away
Swelling that explodes over hours, especially in one leg with new pain or color changes, should be evaluated the same day to rule out a blood clot. Swelling with sudden shortness of breath, chest discomfort, or a sense that you cannot catch your breath is an emergency and needs immediate help.
Redness that is rapidly spreading up the leg, fever, chills, or feeling very unwell suggests infection and should be seen urgently. If you have heart failure or kidney disease and your swelling is worse than usual, or you gain several pounds in a few days, call your clinician to adjust treatment.
Any swelling that is severe, persistent beyond a few days, or accompanied by new weakness, numbness, or difficulty walking deserves a closer look. Trust what your body is telling you and act on it.
Simple steps to ease everyday swelling
When swelling stems from long days on your feet or sitting too long, simple habits can help. Rest with your legs elevated so your feet are above your heart for twenty minutes at a time. While seated, gently pump your ankles and wiggle your toes to encourage blood flow back to the heart.
Stay hydrated and go easy on salty foods, which make the body hold on to extra water. Choose supportive, well-fitting shoes with room in the toe box. If your clinician says it is safe, consider light to moderate compression socks during the day, taking them off at night.
Regular walks, calf stretches, and maintaining a healthy weight all reduce the pressure on your veins and joints. If you have diabetes or nerve changes, check your feet daily for blisters, cuts, or color changes, and let your care team know about any concerns right away.
A friendly final word
Your feet carry you through busy days, family gatherings, and the moments that matter. Paying attention to swelling is a simple way to look after your health. Most causes are manageable, and the serious ones are safest when found early.
If something about your swelling feels different, more painful, or more sudden than usual, do not wait it out. Call your healthcare provider and share what you are noticing. With the right guidance, you can reduce discomfort, protect your circulation, and keep moving with confidence.