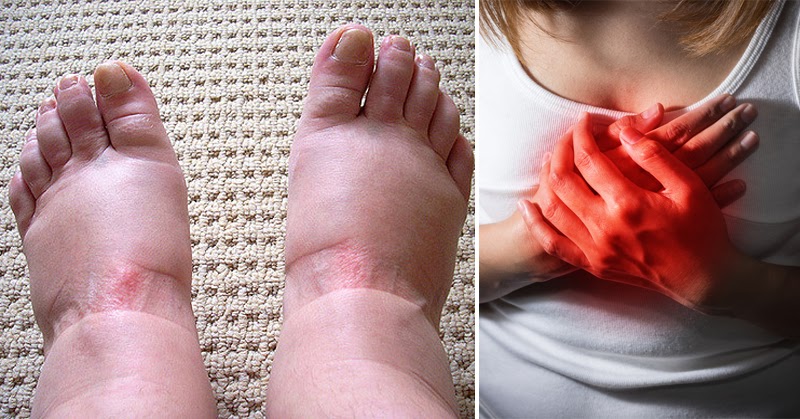
Swollen feet are something many of us notice from time to time, especially after a long day on our feet, a warm afternoon, or a lengthy trip in the car or on a plane. In many cases, that kind of swelling settles down once you put your feet up for a while. But sometimes, swelling is your body’s way of waving a red flag. Knowing when to watch, when to rest, and when to call your doctor can make a real difference—especially if you are managing other health concerns like blood pressure, diabetes, heart, kidney, or vein problems.
If your feet, ankles, or lower legs swell and it doesn’t go away, seems to be getting worse, or comes with other symptoms such as pain, shortness of breath, or a change in skin color, it is always best to take it seriously. The following guide explains nine warning signs you should never ignore, what they might mean, and the simple steps you can take right away to protect your health. The aim is not to alarm you, but to give you clear, friendly information so you can act with confidence.
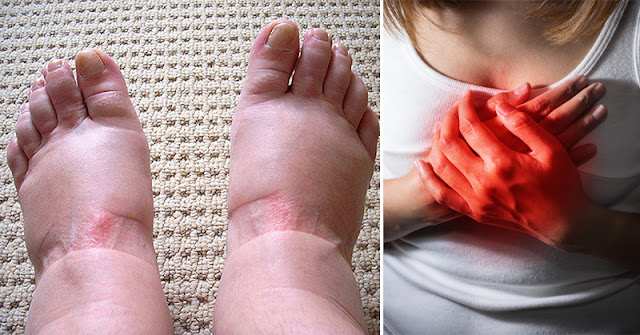
It helps to remember that swelling, also called edema, simply means there is extra fluid in the tissues. Sometimes that extra fluid collects because you have been sitting or standing in one position for too long. Other times, it can be your veins struggling to send blood back to the heart, or a sign that your heart, kidneys, or liver need attention. In more urgent cases, swelling can be connected to a blood clot in a deep vein, called a deep vein thrombosis. That is why paying attention to the pattern of your swelling and any other symptoms that come with it is so important.
Deep vein thrombosis
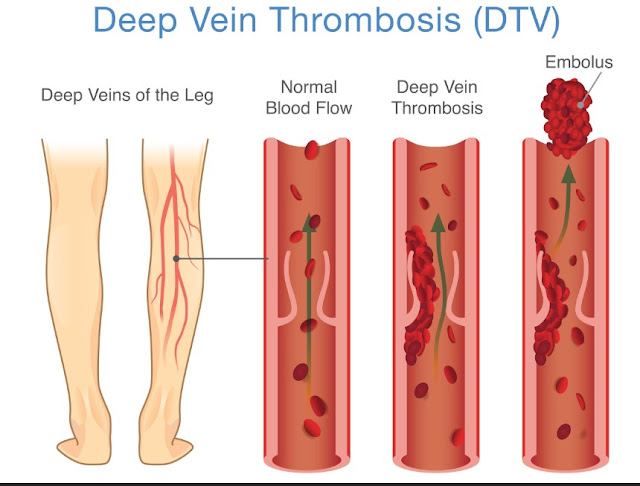
A deep vein thrombosis, often shortened to DVT, is a blood clot that forms in a deep vein, usually in the calf or thigh. While anyone can get a DVT, the risk goes up with age, after surgery, during long travel when you are not moving much, with certain medications, or if you have a history of clotting problems. A DVT needs prompt medical attention because the clot can sometimes travel to the lungs and cause a life-threatening emergency called a pulmonary embolism.
Not all swollen feet mean a DVT, but there are certain clues that raise concern. One of the strongest clues is when one leg becomes noticeably more swollen than the other, especially if it comes on quickly or arrives with pain, tenderness, warmth, or a change in skin color. If you notice a sudden, unexplained swelling in one leg and it does not fade with rest and elevation, reach out to your doctor the same day. If swelling comes with chest pain, sudden shortness of breath, or coughing up blood, call emergency services right away.
Warning sign 1: Sudden swelling in one foot or calf
Swelling that develops quickly and affects just one side is a warning you should not overlook. This kind of one-sided swelling often points to a problem with blood flow in that leg, and a blood clot is one possibility. People sometimes describe a tight feeling in the calf, a heavy sensation, or a sudden change in how their pant leg or sock fits on that side. When this happens without a clear cause such as a recent sprain or injury, it is safer to have it checked promptly. Early treatment, if needed, can help prevent complications and get you back to feeling steady on your feet.
If you are unsure whether the swelling is truly different from your usual, try gently comparing both legs at the same spot, such as the mid-calf or just above the ankle. A clear difference in size, fullness, or tightness that was not there before is a signal to call your healthcare provider. Do not massage a swollen, painful calf, since pressure could potentially disturb a clot if one is present.
Warning sign 2: Pain, warmth, or tenderness along a vein
Pain that feels like a deep ache in the calf, warmth to the touch, or tenderness when you press along the line of a vein can point toward a clot or inflamed vein. Sometimes the skin over the area looks reddish or slightly discolored. If your swelling comes with this kind of tenderness and you cannot link it to a clear cause such as bumping your leg, let your doctor know as soon as possible. In many cases, a quick evaluation and simple tests can rule out a clot and guide you to the right care.
While you wait for advice, it can help to keep the leg at rest and gently elevated on pillows so the heel is slightly higher than the knee and hip. Avoid tight socks or bands around the calf, and make sure you are sipping water regularly unless your doctor has told you to restrict fluids for another reason.
Warning sign 3: Shortness of breath or chest discomfort with leg swelling
Breathlessness that comes out of the blue, chest pain that worsens when you take a deep breath, a racing heartbeat, feeling lightheaded, or coughing up blood are urgent red flags when they happen along with a newly swollen leg. These can be signs of a clot that has traveled to the lungs. This is a medical emergency. Call for help immediately rather than driving yourself. Getting urgent care could save your life.
Even if the symptoms settle before you seek care, you should still be evaluated right away. Treatment for a clot is much more effective and safer when started early, and the right care also helps prevent future problems with the veins.
Warning sign 4: Skin that looks shiny, discolored, very warm, or unusually cool
Changes in skin color or temperature along with swelling deserve attention. Skin that appears shiny and stretched, takes on a reddish, purplish, or unusually pale color, or feels significantly warmer or cooler than the surrounding area can signal trouble. Warmth and redness may suggest inflammation, infection, or a clot. Coolness or a pale color could point to a circulation problem where not enough blood is reaching the foot. If you notice these changes, especially if they are new for you, check in with your healthcare team to be safe.

Make a note of when these changes appeared, what you were doing beforehand, and whether resting with your feet up changes how the skin looks or feels. This information is helpful for your doctor and can guide next steps.
Warning sign 5: Swelling that does not improve with rest and elevation
After a long day, mild puffiness that improves when you put your feet up is usually nothing to worry about. But swelling that stays the same or even gets worse overnight is more concerning. When extra fluid continues to pool in the feet and ankles despite rest and elevation, it can point toward a problem with the veins, the lymph system, or the way your heart, kidneys, or liver are working. If you find that your shoes are consistently tight in the morning or you wake to see your ankles still puffy, it is time to call your doctor for an evaluation.
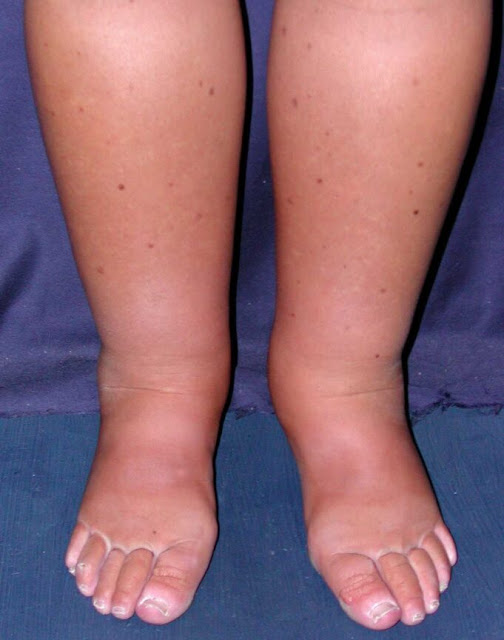
While you wait for your appointment, a few simple steps can make you more comfortable. Try to move your ankles often by pointing and flexing your toes, wear supportive footwear, and avoid sitting or standing still for long stretches. If you use compression socks, be sure they fit correctly and are not too tight at the top. Your doctor can advise you on the right level of compression for your situation.
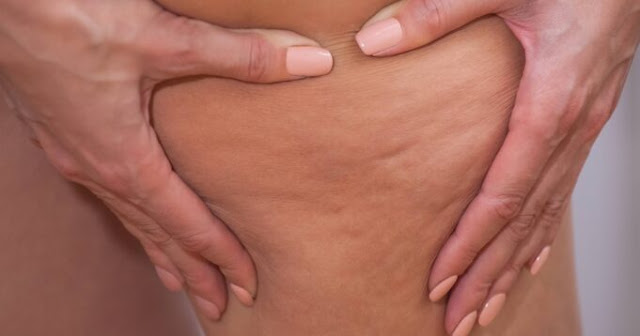
Warning sign 6: Pitting edema or a sudden jump in weight
Pitting edema is when you press a finger gently into the swollen area and a dent remains for a few seconds after you remove your finger. This type of swelling can be linked to heart, kidney, or liver concerns, especially when it comes with a quick gain in weight over a few days. If your rings, waistband, or shoes suddenly feel tighter and the scale shows you are up several pounds almost overnight, it may be extra fluid rather than fat. This is a sign to check in with your healthcare provider, particularly if you already have a heart or kidney condition.
Keeping a small notebook or using your phone to track your daily weight and how your legs look can help you and your doctor spot patterns. If you are following a salt-restricted diet, remember that many packaged foods contain hidden sodium. Cooking more meals at home and tasting your food before adding salt are simple ways to stay on track.
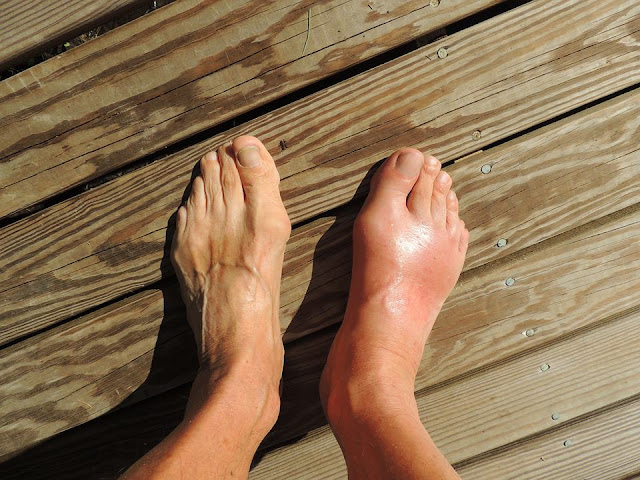
Warning sign 7: Numbness, tingling, or weakness in the toes or foot
Swelling that presses on nearby nerves can cause numbness, tingling, a pins-and-needles feeling, or even weakness in the foot. This is more than just uncomfortable. Over time, reduced sensation can make it harder to feel a blister, a cut, or an area of pressure inside a shoe, which raises the risk of sores and infection. If you notice new numbness or trouble moving your toes or ankle along with swelling, it is wise to seek medical advice. Early attention can help protect the nerves and prevent falls or injuries.
A comfortable pair of shoes with a wide toe box, soft socks without tight bands, and daily foot checks can make a big difference. If you have diabetes or peripheral neuropathy, let your care team know promptly about any new numbness or tingling, since these symptoms may require special attention.
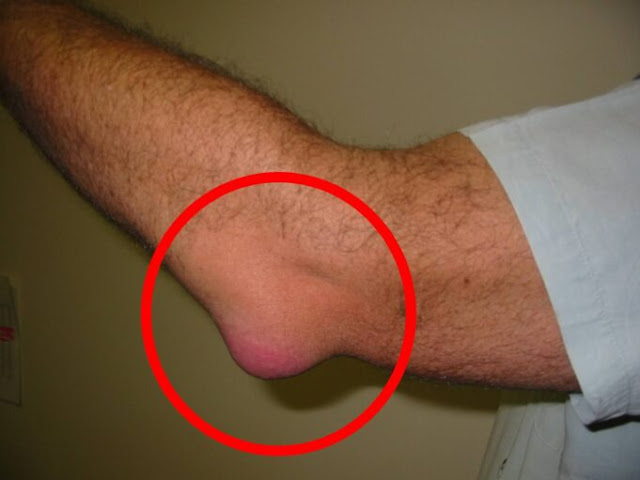
Warning sign 8: Sores, blisters, or signs of infection on swollen skin
Skin that is swollen and stretched is more likely to crack or blister, and any break in the skin is an open door for infection. Keep a close eye on areas where your shoe rubs or where the skin folds at the ankle. Signs of infection include redness that is spreading, warmth, tenderness, pus, or a fever. If you notice these symptoms, contact your doctor right away. Infections of the foot and lower leg need timely treatment to prevent them from getting worse or spreading.
To protect your skin, wash your feet daily with warm water and mild soap, dry carefully between the toes, and apply a moisturizer to the tops and bottoms of the feet, avoiding the spaces between toes where too much moisture can cause problems. Trim your nails straight across to prevent ingrown nails, and consider seeing a podiatrist for regular care if bending to reach your feet is difficult.
Warning sign 9: New swelling after starting a medication or with other health conditions
Some medications can cause swelling, including certain blood pressure pills, anti-inflammatory pain relievers, and hormones. If you notice new puffiness within a few days or weeks of starting a medicine, do not stop it on your own, but do call your prescribing doctor to discuss options. Sometimes a small dose change, switching to a different medication, or adding simple measures like compression stockings can solve the problem.

Swelling is also more likely if you have heart failure, kidney disease, liver disease, or long-standing problems with the veins in your legs. In those cases, monitoring your legs and weight daily, sticking to medication and diet plans, and checking in regularly with your care team are the best ways to stay ahead of fluid buildup.
What to do right now if your feet are swollen
If your swelling is mild and you are otherwise feeling well, try resting with your feet elevated above the level of your heart for 20 to 30 minutes, two or three times today. Gently move your ankles up and down to help your calf muscles pump fluid back toward your heart. Choose supportive shoes and avoid tight socks, garters, or anything that digs into your skin. Cut back on salty foods for a few days and sip water regularly unless your doctor has given you different instructions. These small steps often help temporary swelling improve.
If the swelling is new, severe, on one side only, or comes with pain, color changes, warmth, numbness, fever, or any breathing problems, contact your healthcare provider now or seek urgent care. Trust your instincts—if something feels different or worrisome, it is always better to be checked.
Simple ways to help prevent future swelling
Prevention is easier than treatment. When you know you will be sitting for a while, such as during a long car ride, set a reminder to take quick stretch breaks, flex your ankles, and circle your feet. If you are on a flight, try to get up and walk the aisle every hour. At home, propping your feet up on a small stool while reading or watching television can keep fluid from pooling. If your doctor recommends them, wear properly fitted compression socks during the day, and take them off at night. Keeping your blood pressure, blood sugar, and weight in a healthy range also helps protect your circulation.
Foot care matters. Check your feet daily for any new redness, blisters, or sore spots, especially if the skin is swollen. Moisturize to prevent cracks, keep toenails trimmed, and choose shoes that fit well with enough room for your toes. If you struggle to reach your feet comfortably, it is perfectly reasonable to ask for help or to schedule regular visits with a foot care specialist.
When to call your doctor versus when to call for emergency help
Call your doctor the same day if one leg becomes suddenly more swollen than the other, if the swelling does not improve with rest and elevation, if you notice pitting edema along with a rapid weight increase, or if you see changes in skin color or temperature. Seek emergency care immediately if swelling in one leg is paired with sudden shortness of breath, chest pain, fainting, or coughing up blood. In urgent situations, it is always best to call for help rather than driving yourself.
Your health and comfort are worth protecting. Most of the time, swollen feet are a fixable problem with simple steps at home. But when swelling sends a warning, listening to your body and acting promptly can help you stay active, independent, and well. Keep this guide handy, share it with someone you care about, and do not hesitate to reach out to your healthcare team with questions. Clear information and early action are your best tools.